

Management of a Pregnancy With an Anencephalic Baby
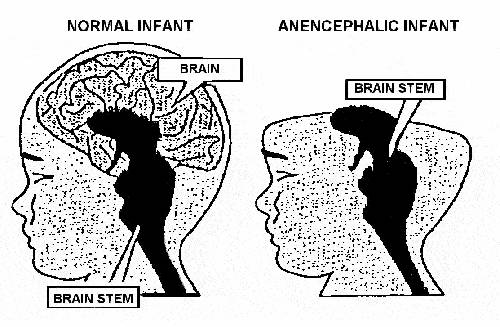
Diagram of Anencephaly
Management of a Pregnancy With an Anencephalic Baby
Professor of Pediatrics Loyola University Stritch School of Medicine
The use of ultrasound to screen pregnancies has led to earlier bonding of parents to their unborn children as they are able to observe the developing child and watch it move early in pregnancy. In addition, however, some defects previously only recognized at birth have been brought to the attention of parents prior to birth as a result of ultrasonic detection. This is particularly true of abnormalities resulting in structural defects such as neural tube disorders. With the ability to recognize anencephaly in-utero, there has developed pressure to induce early labor in order to terminate the pregnancy of the woman carrying the anencephalic child.
Rationale for Intervention
The alleged benefit to result from induction of labor under such circumstances is to relieve the mother of the psychological trauma of having to carry a grossly abnormal fetus throughout the full term of her pregnancy. Presumably the closeness of the Mother-infant bond occasioned by the maintenance of pregnancy would intensify the mourning associated with being the parent of a child with defects. Since early induction of labor was not the standard management of such pregnancies prior to widespread use of ultrasound, there are very limited data as to the real therapeutic benefit of this method of care. The sporadic discovery of anencephalic infants through radiographs taken for another purpose or, more recently, through alpha-feto-protein screening has not provided for sufficient follow-up for evaluation. The recognition of anencephaly either in-utero or in the nursery after birth is unquestionably traumatic for parents. Although the period of time between recognition and the death of the child is usually brief when the diagnosis is made postnatally, the need for support and counseling is much more prolonged. Although conventional strategies have involved keeping the anencephalic infant apart from parents, there is a serious question as to the benefits to be derived from a strategy of denial.(1) Experience with providing support for parents of children with severe defects in general would tend to indicate that there are salutary effects from having parents affirm the reality of their relationship to the child by naming the baby and holding it prior to death.(2) The mourning process when acted out rather than suppressed may be an integral part of ultimate acceptance and healing. Whereas the principal support system for parents of children born with congenital anomalies will typically consist of neonatologist, pediatricians, social workers, geneticists and psychiatrists, the proposal for early induction of labor will usually originate from an obstetrician.
Ethical Considerations
Directive 15 of the Ethical and Religious Directives for Catholic Hospitals (3) states "Every procedure whose sole immediate effect is the termination of pregnancy before viability is direct abortion." The deliberate termination of pregnancy involving an anencephalic child prior to viability would thus be a direct abortion and therefore morally unacceptable. This is so even though the survival of the viable anencephalic child would typically be only 1-7 days. What about the induction of labor after viability but prior to the end of the term of gestation? The dilemma posed by this situation would be somewhat analogous to that of the pregnancy complicated by early rupture of the amniotic sac. Early rupture of the amniotic sac results in an increased risk of infection beginning as an amnionitis or infection of the membranes around the fetus but potentially spreading to result in infection of the unborn child and eventually the possibility of maternal sepsis as well.(4) Although there have recently been inventive strategies for the prevention of such infections by the introduction of sialastic catheters allowing for direct introduction of antibiotics into the uterine cavity,(5) there is substantial risk of infection to mother and child. Induction of labor has been proposed in such cases as the only alternative to potentially fatal sepsis. Induction of labor also poses increased risk for the child related to the various complications of prematurity.
Can such risks be justified using the principle of double effect with the intended good effect of the prevention of infection justifying the bad effect of possible death from premature birth? Since the good effect in this case follows directly from the bad effect that is, it is the early delivery that removes the infant from the infected environment, it is unlikely that the Principle of Double Effect could be legitimately applied.(6)
Early induction of labor in pregnancies complicated by premature rupture of the membranes could be justified if it could be shown that the child was being delivered into an environment where its chances of survival were actually enhanced over the chances of survival in utero. For example, the chances of survival for an infant delivered in high risk centers at 24 weeks gestation were approximately 45%. (7) If it could be demonstrated that 100% of infants will die from infection in pregnancies complicated by prolonged rupture of membranes at 24 weeks gestation, then induction of labor will introduce the infant into the environment of the Neonatal Intensive Care Unit where his survival potential is significantly improved.
Could an analogous justification be constructed for the induction of labor between viability and full term of gestation where the mother is carrying an anencephalic child? The benefit derived is the relief of the anxiety of the mother who is carrying the anencephalic child. The Principle of Double Effect would not apply since the good effect would result directly from the premature termination of gestation with its attendant risks related to prematurity itself. Are these risks relevant when we recognize that the anencephalic child will "die anyway" since its prognosis for prolonged survival after birth would be hopeless even if allowed to go to term? Unlike the infant in the pregnancy complicated by premature rupture of the membranes, however, the chances for survival of the anencephalic infant in the short term are worsened rather than enhanced, The anencephalic infant will survive in utero as long as support is provided through the placental attachment. For the anencephalic infant, however, birth guarantees death (8) since sustained respiratory and cardiac function will be impossible on his own.(9) Induction of labor, in this type of case, guarantees that the anencephalic infant will die sooner rather than later. It is the early death of the infant as well as the separation of the infant from his pregnant mother that is posed as a justification for ending the pregnancy prior to term. The mother's knowledge that the anencephalic child is alive within her is alleged to be the principal cause of her anxiety and the delivery and subsequent inevitable death of the child is proposed as the source of relief from this anxiety.
Devaluation of the Anencephalic Child
There have been recent attempts in the United States and elsewhere to qualify the anencephalic child as an organ donor by reclassifying such infants as "brain absent" and therefore equivalent to "brain dead."(10) One university medical center attempted to implement a protocol to harvest organs from anencephalics by placing them on ventilator support after birth.(11) The protocol was eventually abandoned as unworkable and ethically repugnant.(12) Commentary on attempts to change the laws on determination of death to allow for a special category of "brain absent" for anencephalics has been generally condemnatory in the medical literature in the United States.(13) Bills to legalize declaration of death by virtue of "absence of the brain" have been introduced in at least three states but have not been enacted.(14) Programs for transplantation of organs from anencephalic infants have been approved in Germany, Japan and Holland.(15)
The anencephalic is not truly brain absent of course, since brain stem function is present during the short survival period. Very little is known about neurological function in the anencephalic newborn. A recent in depth study(16) indicates that they are functionally closer to normal newborns than they are to adults in chronic vegetative states.
Evaluations of the status of anencephalic infants in the medical literature are frequently pejorative. To some the issues of life and death are said to be irrelevant since the anencephalic is "uniquely subhuman."(17) One transplant surgeon has classified anencephalics as "non-persons" who will die anyway and therefore are to be preferred as donors to "healthy baboons."(18)
One standard proposed by the American Academy of Pediatrics for medical interventions involving infants is that what is done must be in the best interest of the child.(19) Protocols which recommend termination of pregnancy at any point where the diagnosis of anencephaly is established do not of course, address themselves to the best interest of the unborn anencephalic child. The practice of arbitrary induction of labor will inevitably lead to a further erosion of society's dwindling respect for the status of the anencephalic infant. It will, by extension, undermine the protection of infants with other severe abnormalities particularly those involving the central nervous system (e.g. hydranencephaly, microencephaly, holoprosencephaly).
For those who accept abortion as a legitimate medical procedure there will be no conflict, of course. Anencephaly has been listed among diagnoses justifying the performance of eugenic abortion in the third trimester.(20) Early induction of labor in anencephalics is best understood as a variety of late abortion.
Conclusion
The diagnosis of anencephaly is being made more frequently as a result of routine ultrasound evaluation during pregnancy. Some institutions have instituted protocols for the termination of pregnancy at the time the anencephalic child is ascertained. Induction of labor prior to viability in such instances would be direct abortion. Induction of labor after viability but prior to term would not be in the best interest of the anencephalic child. The purpose of the induction of premature labor would be to relieve maternal anxiety and mourning. In such a rationale, the child in a Kantian (21) sense, is being used as a means to an end. The end is the laudable goal of improving the mental state of the mother and the child's prognosis is hopeless for long term survival. Nevertheless, induction of labor irrespective of the unborn child's best interests will inevitably lead to further devaluation of the anencephalic child in particular and severely deformed children in general.
There is currently insufficient evidence for the therapeutic effect of such procedures. The parents of anencephalic children will need to be provided with long term support and counseling regardless of when the baby is born. Sympathetic and intensive programs of counseling are not precluded by the presence of and continuation of the pregnancy. Further clinical research and evaluation of such programs should be a high priority goal of obstetrical departments. It may be that direct intervention against anencephalic infants may aggravate rather than ameliorate the long range adjustment problems of parents.(22)
Footnotes
1. Zuk, G. H., The Religious Factor and the Role of Guilt in Parent Acceptance of a Retarded Child, Am. J. Ment. Def 64:139, 1969.
2. Fost, N., Counseling Families Who Have a Child With a Severe Congenital Anomaly, Pediatrics 67:321, 198 1.
3. Ethical and Religious Directives for Catholic Hospitals (The Catholic Hospital Association, St. Louis, Mo.) p.4 Second Edition.
4. Naeye, R. & Peters, E., Causes and Consequences of Premature Rupture of the Fetal Membranes, Lancet 1:192, 1980.
5. Giannopoulos J., Unpublished data.
6. LaRochelle, S. and Fink, C., Medical Ethics, Westminster, Md. Newman Press, 1950.
7. Statistics for 1989, Neonatal Intensive Care Unit, Loyola University Medical Center, Maywood Ill.
8. Baird, P. A. & Sandovnick, A.D., Survival in Infants with Anencephaly, Clinical Pediatrics 23:268, 1984.
9. Diamond, E., Anencephalic Infants as Donors for Organ Transplantation, Linacre Quarterly 56:11, 1989.
10. Harrison, M.R., The Anencephalic as an Organ Donor, Hastings Center Report 16:21,1986.
11. Peabody, J., Plan to Use Anencephalic Organs Being Reevaluated, Pediatric News 22.17, 1988.
12. Peabody, J., Frank Admissions End Fetal Organ Harvesting, Los Angeles Times 8-19-88 Page33.
13. Capron, A. M., Anencephalic Donors: Separate the Dead from the Dying, Hastings Center Report 17:5, 1987.
14. California Senate Bill #2018, Ohio Substitute House Bill #718, New Jersey Assembly Bill #3367.
15. Holygreve, W., et. al., Kidney Transplantation in Anencephalic Donors, New Eng. J. Med. 316:1069, 1987.
16. Shewmon, D.A., Anencephaly, Selected Medical Aspects, Hastings Center Report 18:11, 1988.
17. Smith, D. R., The Legal Recognition of Neocortical Death Cornell Law Review 71:850, 1986.
18. Gianelli, D., Pediatric Surgeon Back in the Spotlight with Controversial New Donor, AMA News 11-5-87.
19. Smith, G. F., et. al., The Rights of Infants with Down's Syndrome, J.A.M.A. 2-51:229, 1984.
20. Chervenak, F., et. al. When Is Termination of Pregnancy During The Third Trimester Morally Justified, New Eng. J. Med 310-.501, 1984.
21. Kant, I., Groundwork of the Metaphysics of Morals, New York, Harper and Row 1964.
22. Cooley, W. C., et al Reactions of Mothers and Medical Professionals to a Film About Down's Syndrome, Am. J Dis. Child 144:1112,1990.